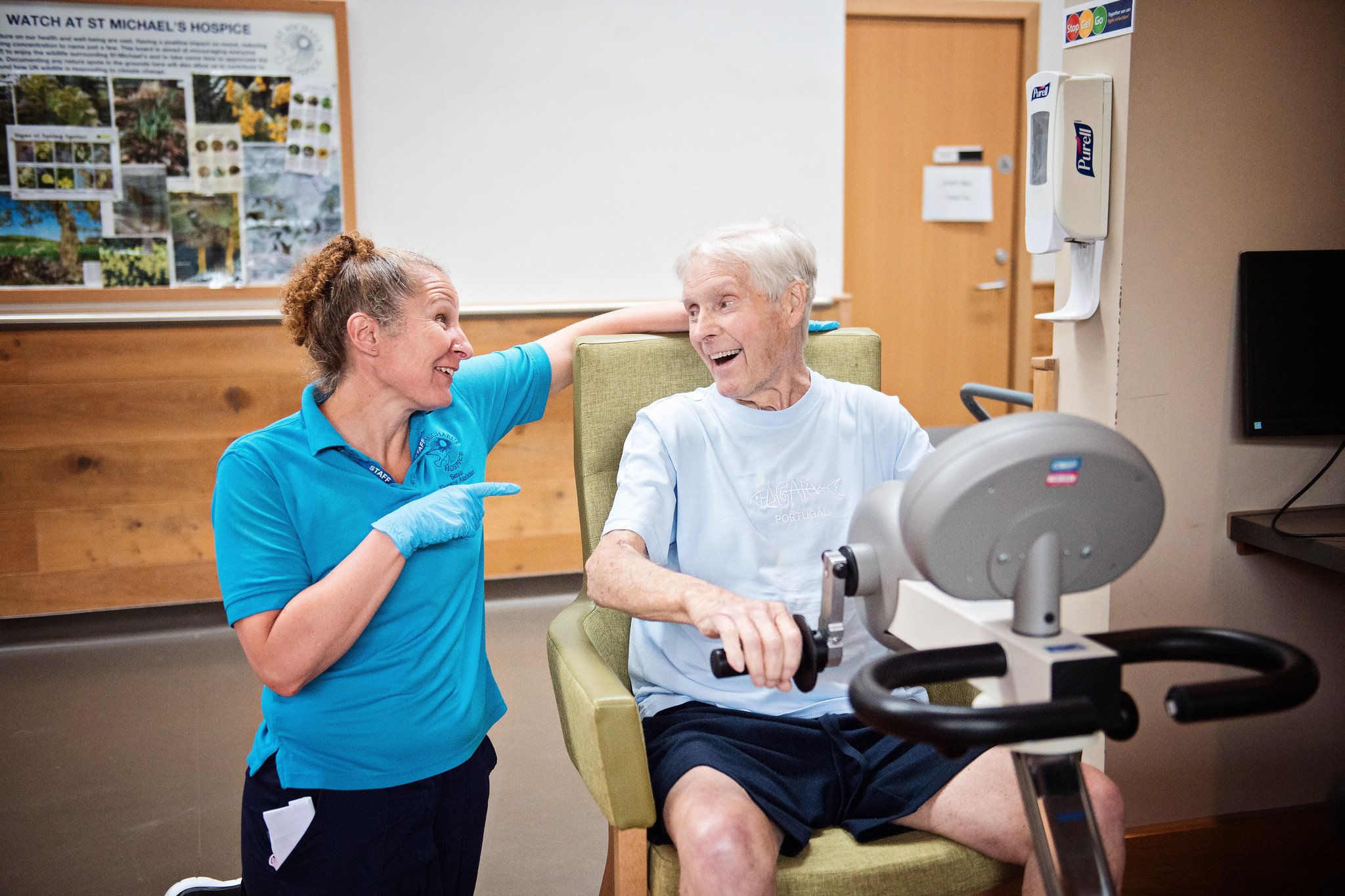
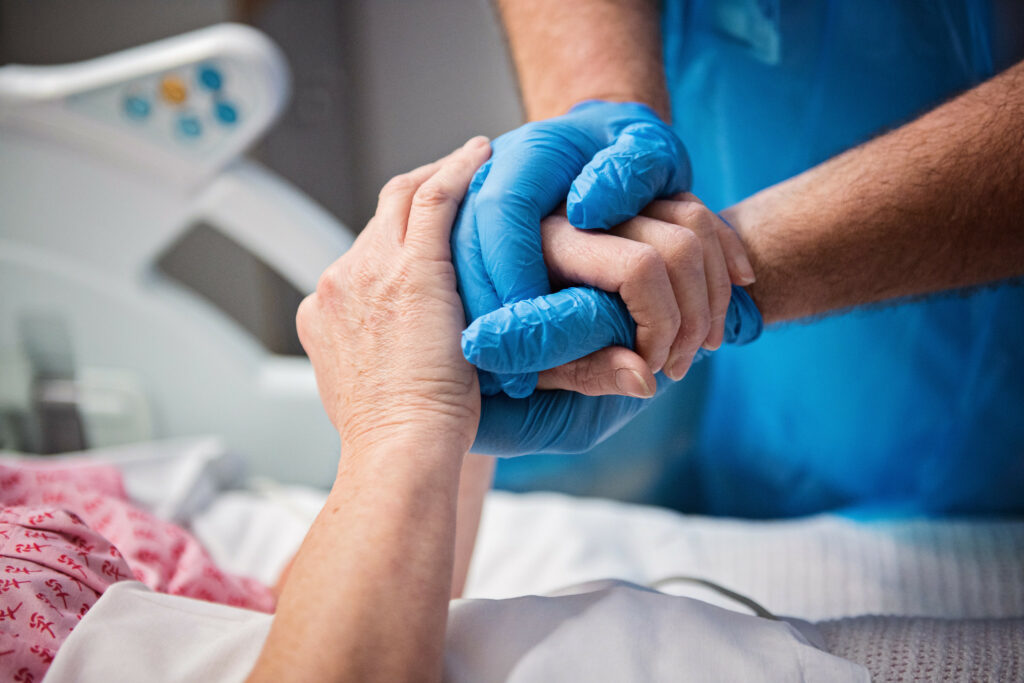
There are 16 private Inpatient rooms within the new Hospice building. Our first-class facilities provide a relaxed and peaceful environment and house 16 large en-suite bedrooms overlooking open countryside and gardens.
Our first-class facilities provide a relaxed and peaceful environment and house 16 large en-suite bedrooms overlooking open countryside and gardens.
Delicious fresh food is prepared daily by our catering team
If you have specific dietary requirements, please talk to a member of staff, and they will make arrangements to meet your nutritional needs.
Every day you will be allowed to order meals from a set menu. A healthcare assistant and a member of the kitchen staff will take your order between 9am and 9.30am for lunch, and between 3pm and 3.30pm for supper and breakfast.
You will be able to choose a cooked meal, salad or sandwiches from the menu. If you do not like anything on the menu, we can offer you an alternative. You can eat our meals in the communal area or your room. Soft drinks are also available throughout the day and aperitifs are offered before lunch.

There are 16 private Inpatient rooms within the new Hospice building
There are five suites of four bedroom bays within the Inpatient Unit, each with its own name; Shire, Nicholas, Clay, Lloyd and Eveson.
Each suite has four large, single, en-suite bedrooms fully equipped for personalised patient care. Each room has a call bell, telephone, television and direct access to the Hospice gardens. Each of the five suites has a communal area offering comfortable seating which can be used for dining, watching television, rest and relaxation.

We can support you
We understand that it’s a difficult time. We are always willing to talk to you to help provide the support and care you may need.
Navigate sections
Ward layout
There are five suites of four bedroom bays within the Inpatient Unit, each with its own name; Shire, Nicholas, Clay, Lloyd and Eveson.
Each suite has four large, single, en-suite bedrooms fully equipped for personalised patient care. Each room has a call bell, telephone, television and direct access to the Hospice gardens. Each of the five suites has a communal area offering comfortable seating which can be used for dining, watching television, rest and relaxation.
Patient meals, special diets, refreshments
Your nutrition is very important to us, and delicious fresh food is prepared daily by our catering team. If you have specific dietary requirements, please talk to a member of staff, and they will make arrangements to meet your nutritional needs.
Every day you will be allowed to order meals from a set menu. A healthcare assistant and a member of the kitchen staff will take your order between 9am and 9.30am for lunch, and between 3pm and 3.30pm for supper and breakfast.
You will be able to choose a cooked meal, salad or sandwiches from the menu. If you do not like anything on the menu, we can offer you an alternative. You can eat our meals in the communal area or your room. Soft drinks are also available throughout the day and aperitifs are offered before lunch.
Relatives’ meals
Hot meals are available in the café. If the café is closed, there are sandwiches and snacks available at all times on request.
Hot drinks can be made free of charge in the beverage bay in the ward area. We also have vending machines with snacks and soft drinks available.
Keeping in contact with friends and family
Mobile phones can be used in the building.
Each room has a bedside telephone (dial 9 for an outside line) which can also take incoming calls from the main switchboard or nursing station.
Your family and friends can also contact a member of staff to enquire about you.
It is helpful for us if one member of the family is elected to make enquiries on everyone’s behalf. Please call the main Reception on 01432 851000 and ask to be put through to the ward office.
Wifi connection
There is free wifi throughout the Hospice. The network you need to connect to is SMH-public. If you experience any problems getting a connection, please do not hesitate to speak to a member of staff.
We are also able to support the use of video calls to enable patients to keep in touch with friends and family.
Discharge Process from Inpatient Unit
We aim to ensure coordinated, safe and timely discharge of patients from the Hospice, ensuring that the appropriate arrangements are in place for ongoing care that continues to meet the needs of our patients and their families.
We will commence discharge conversations early into your admission.
Some people will require very little support from other services after discharge, whereas others may need a full care package.
Unfortunately, due to the high demand for our services, people are not able to live longer-term at the Hospice. This means that if a person’s condition is such that care can be safely provided elsewhere, or if an individual no longer explicitly requires our specific palliative care input, then discharge will need to be considered and planned.
When is discharge considered?
The inpatient unit at St Michael’s Hospice is designed to provide personalised symptom management and restore patient independence as far as their condition will allow.
The discharge process is triggered either:
When a person requests discharge from Hospice services OR
When it is deemed that the patient no longer requires the specialist level of care provided by the inpatient unit at St Michael’s Hospice.
We work together with patients and families to provide personalised care which respects personal wishes. For example, if someone is being cared for at the Hospice but would like to be at home at the end of life, we will work hard to achieve this.
We appreciate that sometimes people would, ideally, prefer to stay in the Hospice.
Unfortunately, due to the high demand for our services, people are not able to live longer-term at the Hospice. This means that if a person’s condition is such that care can be safely provided elsewhere, or if an individual no longer explicitly requires our specific palliative care input, then discharge will need to be considered and planned.
What happens during discharge planning?
During discharge planning, the personal circumstances, needs and wishes of each individual are carefully considered, including any recent changes in condition that may influence the level of care and type of follow-up required.
We use information gained from our assessments to advise on how to best manage the patient’s condition in their preferred place of ongoing care. We might suggest, for example, that our Hospice@Home team or district nurses visit regularly after discharge, that certain equipment might be needed, or that a residential or nursing home may be able to more appropriately meet a person’s specific needs.
In more complex situations, we will hold a meeting with the patient, their family/carer Hospice staff and professionals from other agencies to discuss options and agree discharge plans. If a person’s situation changes during discharge planning, then the decision to discharge may be discussed again and deferred if appropriate.
If extra care is needed at home, or if residential or nursing home care is required, the Social Work Team can advise on how this might be funded.
Who is involved in discharge planning?
The Hospice team provide support and information to enable the patient – and where appropriate their family or carer – to be closely involved with any decision-making about care throughout their time at St Michael’s Hospice and at the time of discharge. We work together to facilitate care packages that are suitable for each individual.
Several members of the Hospice team may be involved in supporting discharge planning, such as the nurse, doctor, physiotherapist, occupational therapist and social worker.
The Hospice team also works closely with other teams in the community and in local hospitals. These professionals often need to be involved in the discharge planning process and can become further involved with a patient after discharge, eg, Hospice@Home, community nurse specialist, district nurses, physios and occupational therapist. They may continue to monitor a person’s condition alongside the GP, or may continue to offer specific interventions for problems such as lymphoedema, catheter care or wound care.
What happens at the time of discharge?
Any person discharged from Hospice services is given information about who to contact if there are any problems, including the
24 hour Hospice Advice Line on 01432 852080.
Information is also provided about follow-up arrangements and a discharge letter is sent to update other professionals involved in the patient’s care, such as the hospital consultant or specialist nurse, GP, district nurses and out of hours services, such as Hospice@Home.
Everyone discharged from the inpatient unit is given an appropriate supply of medication – to allow enough time to order a repeat prescription from their GP – as well as an information sheet about the medication.
What can be done if a person’s condition changes after discharge?
By working together, we hope to meet the needs of each individual and their family/carers, whilst ensuring our services are open to as many people as possible.
However, we also know that sometimes people need us again at a future date. If the need arises, a professional (such as the GP, District Nurse, Community Palliative Care team or Consultant) can refer a patient back to Hospice services.
Make a referral
Patients can be referred to the Hospice either by their GP, community nurse specialist, district nurse, hospital doctor or consultant.
The Hospice’s tranquil setting cannot be underestimated. It’s miles away from the frenetic hubbub of everyday life. Here, I have been able to relax and spend my mornings watching the sunrise. It does wonders for the soul